Introduction:
In glucose clamp experiments, variable glucose infusion rates (GIR) are used to control blood glucose concentration (BG, the ‘physiological variable’) and keep it close to a fixed target level. You can find more information about clamps here.
As no control algorithm will result in a perfect, flat BG curve (always being at target), BG will show some dynamic behavior, which can be used to describe the quality of glucose clamps. In a glucose clamp with good quality the BG variability (‘precision’) as well as the mean deviation from target level (‘control deviation’) are low. You can find a description of clamp quality parameter here.
However, control deviation (CD) might overestimate glucose clamp quality as periods with BG above target might be offset, at least partly, by periods below target. This limitation does not apply to absolute control deviation (aCD): 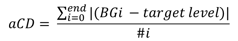
The figure below schematically shows the dynamic BG behavior (red) for two different glucose clamps using different clamp algorithms.
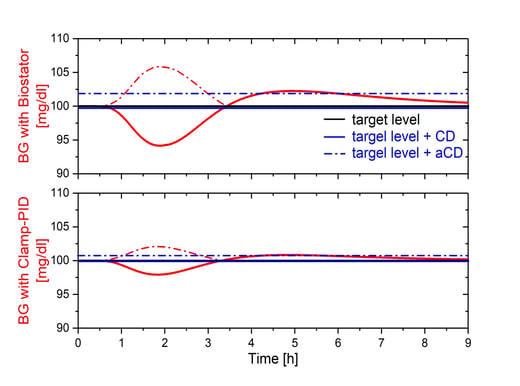
The well-established Biostator algorithm [1] used in the top panel leads to a BG-drop at around 2h and prolonged BG values above target level starting at 3.5h. BG values obtained with the new Clamp-PID algorithm [2], optimized for rapid and ultra-rapid insulins (see more information to new PID-algorithm here), shown in the bottom panel are much closer to target level, i.e. this glucose clamp has a better clamp quality than the above one. Nevertheless, control deviation of both algorithms are both close to zero i.e. mean deviation from target level is very small (solid blue lines). Large negative deviations from target level at the beginning of a clamp are nullified by later positive deviations.
To overcome this disadvantage aCD takes absolute deviations from the target level into account. That leads to a larger aCD for the Biostator algorithm than for the Clamp-PID algorithm (dashed blue lines). aCD is therefore much better suited to describe the quality of glucose clamp control algorithms to keep BGs stable and close to target.
Methods:
We conducted a small cross-over study in 5 healthy subjects who received 0.3U/kg of fast acting insulin aspart (NovoRapid, Novo Nordisk, Bagsvaerd, Denmark) on two different study days under euglycemic glucose clamp conditions (ClampArt, clamp level 81 mg/dl, clamp duration 12 hours post-dosing). Two different clamp algorithms (Biostator algorithm and a new Clamp-PID algorithm) were used in random order to determine GIRs.
Absolute control deviation and the other established clamp quality parameters were derived for all clamps. Data were not corrected for any implausible BG values due to clotting, movement, etc. Clamp quality parameters were analyzed for two-hour intervals and over the whole clamp duration.
Results:
We calculated CDs for 2-hour intervals of the two clamps in order to prevent a nullification of deviations below target at the beginning of the clamps through deviations above target later in the clamp.
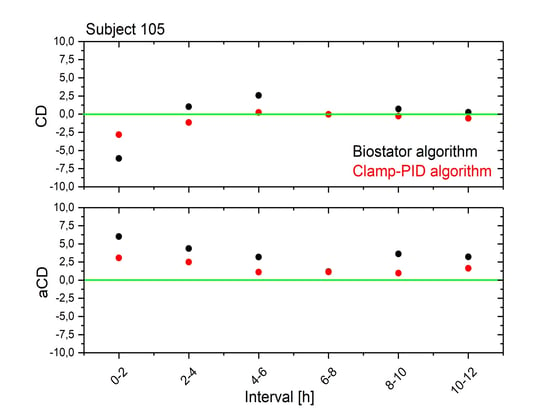
CD for Clamp-PID algorithm was closer to zero than CD for the Biostator algorithm for nearly all 2-hour intervals. However, almost all CD-values for the Clamp-PID algorithm were negative, as was the overall CD for the total clamp duration. Deviations with the Biostator algorithm were both positive and negative and therefore close to 0 when they were combined to a total value. The advantage of the Clamp-PID algorithm (closer to target level in each 2h interval) disappears in the total value.
In contrast, aCD results for 2-hour intervals are positive and did not nullify each other as shown in the figure above. Similar to CD, the aCD values for the Clamp-PID algorithm are closer to target level in each of the 2-hour intervals, but because all values are positive, the combined total aCD is clearly smaller when using the Clamp-PID algorithm compared to the Biostator algorithm.
The following table shows the mean results (±SD) of all five subjects for both the individual 2-hour intervals and the complete clamps.
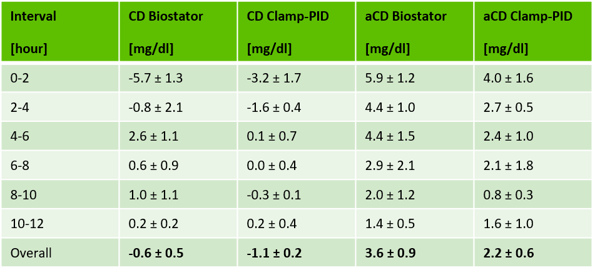
While the Clamp-PID algorithm showed CD-values closer to zero in almost all intervals when compared with the Biostator algorithm, the overall CDs were quite similar (-1.1mg/dl ± 0.2mg/dl with the Clamp-PID versus -0.6mg/dl ± 0.5mg/dl with the Biostator algorithm).
In contrast, the lower aCD-values with the Clamp-PID algorithm in all, but the last 2-hour intervals also leaded to substantially lower overall values versus those obtained with the Biostator algorithm (2.2mg/dl ± 0.6mg/dl vs. 3.6mg/dl ± 0.9mg/dl).
Conclusion:
The clamp quality parameter ‘control deviation’ might misleadingly indicate almost perfect clamp quality when negative blood glucose deviations from the target level are compensated by blood glucose concentrations above target. ‘Control deviation’ as clamp quality parameter should therefore always be combined with ‘precision’ as a parameter of blood glucose variability. This limitation of ‘control deviation’ is overcome by the new clamp quality parameter ‘absolute control deviation’, which describes absolute deviations from target level.
The introduced quality parameter is well suited to compare clamp results. We therefore determined the new clamp quality parameter ‘absolute control deviation’ and the established quality parameters retrospectively for clamps investigating prandial and basal insulins conducted at Profil between 2014 and 2019.
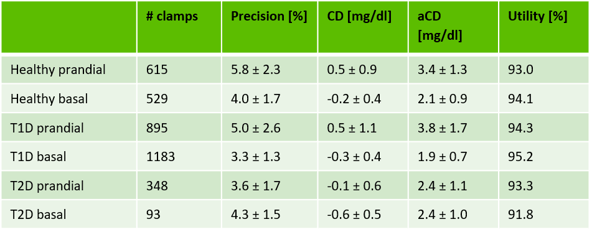
Results for ‘control deviation’ varied around null for prandial as well as basal insulins whereas ‘absolute control deviation’ showed differences according to used insulins. ‘Absolute control deviation’ showed smaller values in clamps with basal insulins than in clamps that investigated rapid- or ultra-rapid-insulins. This directly correlates with ‘precision’: larger ‘precision’ in clamps with prandial insulins leads to larger ’absolute control deviation’ while better (i.e. smaller) ‘precision’ in clamps with basal insulin results in better ’absolute control deviation’.
Read more about our expertise in testing medical technology: Insulin pump development and design, artificial pancreas study and the AP@home project, glucose monitoring.




