A Remote Decentralised Clinical Trial (RDCT) design can be a valuable option to make your clinical trial more efficient. Also called web-based or hybrid trials, they combine digital technologies with more “conventional” design elements to bring clinical research to patients’ homes [1]. RDCTs democratize the access to clinical trials by reaching population groups that would normally not have the possibility to enrol in a clinical trial. Web-based communication paths facilitate the participation of elderly, frail, disable people and people living in remote areas.
RDCTs may help achieving higher levels of sustainability, resilience and external validity in pivotal clinical research.
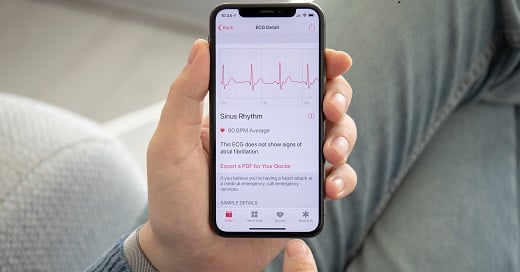
Paradigm examples: AP@home, TELESAGE and Apple Heart Study
The AP@home study is a landmark real-world clinical trial that integrated RDCT design elements to the field of diabetes. The study was a key milestone of the pan-European AP@home project led by Profil and the Academic Medical Center Amsterdam. Results published in the New England Journal of Medicine [2] have shown that it is safe and effective for patients with type 1 diabetes to administer their insulin at home using an automated insulin delivery (AID) system, also named artificial pancreas (AP). The study was setup as a multicentre and multi-national randomised controlled clinical trial. Notably, participants performed their usual everyday activities under free-living conditions, even without continuous remote monitoring or supervision. They were completely free to choose their meals and all of them had access to a 24/7 helpline.
The TELESAGE (Suivi a Grande Echelle d’une co-horte de diabétiques de type 1 et de type 2 sous schéma insulinique basal bolus par la telemédecine) study is a French real-world evaluation of DIABEO® which was set up by the Centre for Studies and Research for the Intensification of Diabetes Treatment (CERITD). DIABEO® is a digital health application that supports patients with diabetes on their insulin therapy and connects them remotely to their attending diabetes teams [3]. The study has shown that the use of DIABEO® is safe and improves glycemic control. Given its large size, the study was able to identify factors that predict the use of DIABEO® and the achievement of a better glycemic control under everyday living conditions [4]. During the study, a diabetes logbook, a bolus calculator and an auto adaptive algorithm calculating the adjustment of basal insulin were connected to a mobile app. Healthcare providers had access to a web portal containing a remote treatment configuration module and tools providing coaching and feedback on a per-patient and per-physician basis [5].
Having enrolled more than 400.000 participants, the Apple Heart Study is one of the largest RDCTs designed to identify cardiac arrhythmias [6]. This longitudinal observational study was sponsored by Apple and conducted in cooperation with the Standfort Center for Clinical Research and Quantitative Science Unit. The goal of the trial was to assess the suitability of a smartwatch program using an algorithm for photoplethysmography-based detection of atrial fibrillation and to estimate the diagnostic yield in a large population in the US under everyday conditions [7]. The data collected support the view that a photoplethysmography-based detection of pulse irregularities might improve the chances of a timely diagnosis and treatment of previously unrecognised heart disease.
Pan-European RealWorld4Clinic Initiative
Profil, together with other organisations, has launched the pan-European RealWorld4Clinic initiative funded by the European Union [8].The consortium behind this initiative is developing a medical device using a new generation of sensor technologies. A multi-sensor system enables remote acquisition of a wide array of cardiorespiratory health parameters for an AI-powered derivation of digital biomarkers, and it is connected to a smartphone-based communication platform. The platform uses conversational AI, which enables digital assessment of patient-reported outcome measures. Key design features include the seamless connectivity and interoperability with different data sources, a dynamic and fine-grained consent management, as well as the provision of privacy-preserving data access, secure hooks to external algorithms and access to Audit logs and pre-built compliance services.
The goal is to provide cutting edge sensor, communication and data management technologies making the RDCT design fit for usage in pivotal clinical research. Outcome predictors and performance indicators will help to optimise the impact of RealWorld4Clinic on the cost-efficiency and sustainability of clinical trial operations. We firmly believe that RealWorld4Clinic will lead to a high acceptance of RDCTs in pivotal clinical research, clearly beyond merely meeting the mandatory regulatory and legal standards.
Opportunities of RDCTs
RDCTs provide many opportunities compared to conventional clinical trials, especially regarding patient recruitment and enrolment. Study apps provide all relevant information regarding a clinical trial to people willing to enrol in a study. After reading the subject information and consent form, patients can send their registration online or use the app to contact a member of the study team to clarify possible doubts. A study app could also add value to early phase clinical trials by expanding the recruitment of trial participants, facilitating their informed consent, enhancing adherence to clinical trial protocols, supporting the performance of virtual visits and promoting the collection of patient-reported outcome measures. In phase III and post marketing surveillance (phase IV) trials [9] the app-based communication also enables a massive recruitment of trial participants in a short time and at low costs.
Hybrid trials could also enhance cost efficiency in phase I and phase II clinical trials. The implementation of RDCT design elements could improve the quality of sponsor’s early go/no-go decisions regarding the later, more cost-intensive phases of the clinical development program. The availability of real-world data could increase the predictive power and thus the external validity of trial outcomes, thereby boosting the efficiency of clinical development programs by reducing the attrition rates for new drugs and devices.
In multicentre studies, the advantages of RDCTs include a significant reduction in numbers of study centers participating in the trial (e.g. only one centre per participating country) and subsequent decrease in costs. During a RDCT as many trial assessments as possible are carried out in the participant’s life settings, without the need of visiting a medical facility. Indeed, RDCTs aim to reduce the number of in-persons visits to a minimum, and in their extreme form, to avoid completely these visits.
The increased availability of remote monitoring tools and wearables proven to be “fit for purpose” in the specific “context of use” [10] allow for such decentralised and remote approach. Medical-grade wearable devices (optimally interoperable with the study app) can be applied to collect integrated information on digital endpoints based on a (multi)sensor-based acquisition of physiological and behavioural data [11]. Surveys on behaviour patterns, patient-reported outcomes, as well as safety and tolerability issues can be conducted via the study app. For the sampling and processing of biological specimens self-test kits can be shipped to the trial participants. More technically demanding and invasive procedures continue to be carried out by medically trained personnel such as local physicians or study nurses who visit the trial participants at home.
Limitations and risks
During the trial planning activities, a catalogue of multi-dimensional criteria should be applied to each RDCT to achieve a good balance between opportunities, limitations and risks. The strength of a RDCT may depend on the overall objective of the trial and the disease and intervention to be investigated.
Special attention should be paid to: inclusion and exclusion criteria, expected sample size, invasiveness of intervention and assessment procedures, and safety and tolerability profile of a drug or digital health application under study. It should also evaluate the availability of fit-for-purpose remote monitoring devices validated in the specific context-of-use, as well as the readiness to integrate participatory education & training, motivational and feedback tools to determine the opportunities, limitations and risks of a specific RDCT.
A “site-less” workflow that, to a considerable extent, relies on the use of digital communication and assessment tools also carries risks regarding the quality of trial outcomes. The lack of physical contact of trial participants with the study site may affect engagement, adherence to the trial protocol, completeness of follow-up and reliance on participant reported outcomes. Considerable loss of follow-up may account to uncertain validity and generalizability inherent to the RDCT design. There may be a bias due to the preferred inclusion of technology-oriented trial participants and those who have certain communication technologies already available. In case you decide to go for an observational study the RDCT design could even reinforce this bias by adding further (un)known confounders. Overall, there is a risk of RDCTs to unconsciously produce biased results that cannot be fully transferred to patient population targeted by a drug or medical device developer.
Although RDCTs provide many advantages for late phase clinical research, its application in early phase clinical trials is limited. It can still be used for patient enrolment and virtual extra monitoring but in-person visits cannot be completely excluded.
Conclusion
RDCTs may facilitate the continuous collection of real-world data of a high number of trial participants. This could help to better capture the impact of treatment effect modifiers on trial outcomes, thereby narrowing the efficiency gap seen in “conventional” clinical trials (E2E gap) [12]. While conventional trials normally enrol more homogenous groups of participants and are undertaken in well-controlled conditions, RDCTs allow the enrolment of different patient groups and the collection of data in real-world settings.
In addition, early acquisition of insights about treatment effect modifiers in the course of a study could inform readjustments in the trial design. If it turns out that RDCTs actually narrow the E2E gap, the outcomes of such trials could greatly support companies to negotiate attractive contracts with value-based healthcare providers using pay-for-performance-based remuneration.
Integrating the use of medical-grade wearables for a continuous monitoring of physiological and behavioural parameters under everyday conditions holds the promise of collecting real-world information about safety and tolerability and effectiveness of tested drugs and devices. This approach could inform medical investigations outcomes that still need to be scheduled in the clinical research unit.
However, to what extent RDCTs could affect the sustainability and the ecological footprint of clinical research is currently unknown, but that would be a topic for a highly exciting field of research.
RealWorld4Clinic (Real-World Cardiorespiratory Health Monitoring for Clinical Contract Research & Tele-cardiology) is part of the competitive innovation project portfolio funded and curated by EIT Health. EIT Health is funded by the European Institute of Innovation and Technology (EIT), a body of the European Union that receives support from the European Union´s Horizon Europe Research and Innovation programme.
Profil (coordinator), Profil Mainz, SentinHealth, Fraunhofer Institute for Toxicology and Experimental Medicine, University Grenoble Alpes, Inserm, RWTH Aachen, RWTH Aachen University Hospital, CHU Grenoble Alpes, CHU de Rennes, Grenoble Ecole de Management, MADoPA, Zana Technologies, PrYv, aQua Institute, SurgiQual Institute, LINQ management




